Therapies, Interventions and External Professionals
New Siblands has access to a wide range of therapies and interventions. These enhance both the educational and the personal development of the child in a holistic way.
The Therapies and Interventions Lead at New Siblands is Alice Maggs
You can find out more information about the full range of interventions that we offer our young people by clicking to expand the boxes below.
Arts Therapies
The Arts Therapies service is a team of 10 HCPC registered art therapists and an assistant who is based with the Bristol Adult Community Learning Disabilities Teams, but also provide Arts Therapies to children and young people who have moderate to severe learning disabilities in Bristol and South Gloucestershire. The organisation who employs the creative therapists is Sirona Care & Health.
Arts Therapies work through art, drama or music to help children express and explore their feelings, working verbally and non-verbally. They aim to build a safe and trusting psychotherapeutic relationship where the child or young person can feel able to share their thoughts, and work through troubling issues. The content of sessions is confidential but they liaise with teachers, mentors, parents or carers to share general themes arising from the work.
Through the Art therapy process we aim to do the following
-
to provide a safe space for expression of feelings
-
to enable exploration and understanding of feelings
-
to alleviate distress caused by difficult feelings
-
to increase self-esteem and confidence

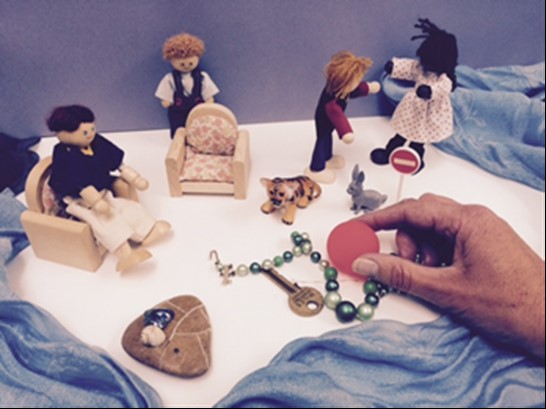

Arts Therapies Referral Process
-
In the first instance, speak with your child's class teacher or contact Krissy Emery (Mental Health Lead).
-
The class teacher will complete the Arts Therapies referral form.
-
Referral form will be sent securely to the Arts Therapies Team Lead.
-
The referrer will be contacted within 8 weeks of receiving the referral.
-
If the referral is accepted, a therapist will call the referrer to discuss the referral. They will make appointments to meet with parents or carers, teaching staff and the young person, and speak to any other involved professionals.
-
During the visits and discussions the therapist will gather information about the young person. This will help them to assess the need for therapy, decide which of the three therapies would be most helpful and give support and advice to parents, carers and professionals.
-
If the young person is offered a Arts Therapy they will wait for a therapy slot to become available before beginning assessment sessions.
-
A risk assessment of the young person and the room to be used for therapy is completed by the therapists in collaboration with the teacher. This will be reviewed as necessary where there are any changes.
-
When therapy begins it will often take place at school. The young person will be offered 6 assessment one-to-one therapy sessions. As the end of the sessions a review will take place to see if therapy proves helpful.
-
If the therapy is helpful for the young person, they will be offered time limited or longer ongoing therapy. If therapy is not helpful we will look for other services who can support them.
-
When the young person is having therapy the therapist will have regular contact with school and home. The need for continuing therapy will be reviewed as necessary.
-
A report will be written by the therapist at the end of the block of sessions. This can contribute to the young persons EHCP and Annual Review.
Emotional Literacy Support Assistant (ELSA)
Mary Rose is an Emotional Literacy Support Assistant (ELSA). She runs ELSA sessions every Friday afternoon for pupils that staff and parents feel will benefit from ELSA interventions.
An ELSA, will work with students who may need additional support with their mental health and well-being.
Some areas they can help with are the following:
- Loss and bereavement
- Self-esteem
- Social skills
- Emotions
- Friendship skills
- Anger management
- Behaviour
- Anxiety
- Bullying
- Conflict
- Relaxation techniques
To support this need, the ELSA will plan activities alongside a learning objective.
The learning objective will be something the student will be able to do at the end of the sessions that they couldn’t necessarily do before the sessions began. For example, Mary Rose may work with a student that will be asked to identify six of their strengths, which is a self – esteem objective. By the end of the session, we would aim for the student to be able to recognise various positive qualities about themselves. The benefit of this is that the student will then recognise the skills that they have and therefore their sense of self-worth and overall emotional wellbeing will increase.
Students are then able to make progress in a variety of curriculum areas and are much happier in school if their emotional needs are supported.
The sessions range from 20 to 45 minutes long and run for 6-8 weeks.
The session consists of the following:
- Emotional check in
- Main activity
- Relaxation
Please click the link to view the leaflet about ELSA
ELSA Referral Process
-
In the first instance, speak with your child's class teacher or contact Krissy Emery (Mental Health Lead)
-
If ELSA is deemed appropriate, the class teacher will liaise with Krissy Emery to fill in the SEMH Triage referral form.
-
Krissy Emery will meet with the referrer to discuss the referral. The referral will then be triaged
-
Krissy Emery will liaise with the ELSA to see when it is appropriate for the input to commence.
-
If the therapy is helpful for the young person, they will be offered time limited or longer ongoing therapy. If therapy is not helpful we will look for other services who can support them.
-
When the young person is having therapy the ELSA will have regular contact with school and home. The need for continuing therapy will be reviewed as necessary.
-
A summary will be written by the ELSA at the end of the block of session. This can contribute to the young persons EHCP and Annual Review.
Aquatic Therapy
Hydrotherapy or Water Therapy, is a complimentary therapy that uses water for health purposes.
It supports muscle strength, independence and opportunity to weight bear.
Pupils eligible are given the opportunity to have a 30 minute weekly slot in the pool,. The physiotherapist carries out an assessment and writes a programme of exercises or activities for a child, this is a reviewed at intervals. Children are supported either 1-1 or 2-1 to undertake their individualised programme. We have 3 members of staff who are dedicated swimming ladies. These are Jodie, Jenny and Louise and on occasions they have Rosie supporting as well.
The 4 key features that make hydrotherapy an effective therapy are:-
- Buoyancy – Aids balance, reduces pain and supports bodyweight whilst strengthening the muscles.
- Water Resistance – Builds up their strength level.
- Hydrostatic Pressure - Pressure on the body helps relieve tightness and reduce swelling.
- Water Temperature – Eases the mind, relaxes muscles and relieves anxiety.
Hydrotherapy exercises can help students to improve their:-
- Oral motor skills and respiratory control – by blowing bubbles, or blowing a lightweight object along the surface of the water.
- Muscle strength – Activities using a water noodle can build muscle in the arms and core without it being obvious to the pupil.
- Concentration and confidence, reducing overall anxiety and stress.
Occupational Therapy
At New Siblands, we currently employ an Occupational Therapist to work collaboratively with the teaching staff, health or social care staff and other therapists across the school.

This is Kathryn Irvine
Occupational Therapy focuses on how motor, sensory, cognitive and emotional skills can affect a child’s ability to participate in activities of daily living with a focus on a functional difficulty.
Kathryn works closely with staff to ensure that our children are enabled to participate in occupations which may include: areas of self-care (e.g. eating a meal); areas of productivity (e.g. engaging in learning); and leisure (e.g. playing).
The input can range from completing short observations of the child participating in activities and making basic recommendations (e.g. doing hand warm ups prior to fine motor tasks or providing a child who is sensitive to sound with ear defenders), to completing assessments and devising individualised recommendations and programmes to support their learning.

All involvement is made in conjunction with the teaching team to adjust and adapt classroom environments and routines.
Basic Occupational Therapy and individualised recommendations and programmes are shared and discussed with parents.
A young person at New Siblands School may also see different Children’s Occupational Therapists for other reasons:
- A Community Children’s Occupational Therapist for advice around self care such as toileting and eating. They can look at supportive seating within school to enable the child to access their learning and to help maintain a good posture. The dedicated therapist is Kate Openshaw.
- A Social Services Occupational Therapist for home equipment needs and adaptations.
Occupational Therapy Referral Process
-
In the first instance, speak with your child's class teacher or contact Karen Miller (Behaviour and Sensory Intervention Lead)
-
The class teacher will complete the relevant Occupational Therapy referral form and return to Karen Miller.
-
Karen Miller will meet with the Occupational Therapists to discuss the referral, add to their caseload and work out when is appropriate for the input to commence.
-
At the beginning of their input, the therapist will carry out observations, gather information about the young person, liaise with with parents or carers, teaching staff and the young person, and speak to any other involved professionals.This will help them to assess the need and provide appropriate strategies and recommendations to school, parents and carers.
-
The Occupational Therapist will review the strategies and recommendations that have been provided after allowing a period of time for them to be implemented and trialled.
Off The Record
OTR’s Wellbeing Practitioners will work with your students between the ages of 11-18 struggling with low-level/mild to moderate common mental health difficulties (stress, anxiety, low mood, sleep problems and behavioural difficulties) working on a journey towards a better wellbeing.
They can help develop a toolkit that helps identify thoughts, feelings and behaviours that may be getting in the way of feeling good. By setting achievable goals together they can help empower young people to make the changes they want.
They can offer this type of therapeutic support in a
number of ways:
• Individually
• Group setting
• Parents/Family
• Face-to face
• Telephone
• Online
OTR has the advantage of being flexible with session times ranging from 15- 45minutes, meaning the Wellbeing Practitioners can hold a larger caseload of students than ever before. Support from the flexible wellbeing team can be as flexible as a one-off session or up to 8 sessions.
Please click the link to view the leaflet about Off The Record
This is Jacob Cunningham who visits New Siblands during the academic year offering 1-1 mental health support.
Hello, my name's Jacob and I'm a Wellbeing Practitioner. If you're feeling worried, anxious or stressed, or you find yourself feeling sad or low a lot of the time then I might be able to help! I will help you work out why you're struggling, and we can work together to find the right support for you, as we all need help now and then. I also use Cognitive Behavioural Therapy (CBT for short), which helps you understand the links between your thoughts, behaviours and feelings and how to make positive changes.

Off The Record Referral Process
-
In the first instance, speak with your child's class teacher or contact Krissy Emery (Mental Health Lead)
-
If input from Off the Record is deemed appropriate the class teacher completed the SEMH triage form.
-
Krissy Emery will meet with the referrer to discuss the referral. The referral will then be triaged.
-
Krissy Emery will liaise with the appropriate professionals to see when it is appropriate for the input to commence.
-
If the therapy is helpful for the young person, they will be offered time limited or longer ongoing therapy. If therapy is not helpful we will look for other services who can support them.
-
When the young person is having therapy the therapist will have regular contact with school and home. The need for continuing therapy will be reviewed as necessary.
-
A summary or report will be written by the therapist at the end of the block of session. This can contribute to the young persons EHCP and Annual Review.
Pet Therapy
Freddie the Dog and Hannah the dog.
These dogs visit New Siblands school with their owners on a weekly basis for a short period of time. The dogs work with children in small groups with supporting adults from the various pupil classes.
These dogs are gentle and loving with impeccable temperaments, but at the same time are full of fun and enjoyment for the children. There are many benefits for pupils working with the dogs. These include: motivating pupils to engage in an activity where they have opportunities to work on their communication and language development, responsibility for walking and grooming the dogs, and relieving anxiety whilst increasing confidence with dogs.
Children can learn to overcome their fear of animals and grow in respect and appreciation for them.
During the academic year, an identified group of pupils work on specific targets with the dog. These targets are usually linked to communication and language, for example pupils give instructions using their preferred mode of communication and follow requests working with the dog.
There is also an identified group of pupils who participate in a sensory session with the dog. They can also work on communication, sensory and physical development by reaching out, touching, smoothing the dog and tracking movements.
Physiotherapy and Clinics
Physiotherapy focuses on how muscles, joints and pain can affect physical skills, posture and walking leading to a functional difficulty.
Physiotherapy is delivered by setting joint goals with parents and/or school. Therapy programmes are then set to meet these goals.
Physiotherapists also assess children for supportive standing and walking equipment where it is required.
We currently have two Physiotherapists working collaboratively with the teaching staff across the school. They also have an assistant to support them with their work at School.

This is Sarah Padwick, Physiotherapist

This is Jade Harris, Physiotherapist

This is Beth Carley,Assistant
The Physiotherapists like to work collaboratively with parents and invite you to contact them to arrange a convenient time to meet at school, home or Patchway Hub (or virtually) to review your child’s strengths, progress and needs together. Their contact details can be found below
Physiotherapy Referral Process
- You can either call the physiotherapy advice line on: 07917393196 between 9 and 12 on a Thursday morning or you can put a referral in, referral forms can be found on the CCHP website, these referrals will be triaged, and a decision will be made at triage whether it is thought a physiotherapist could support your child or not. (NB if you call the advice line, and it is thought that a referral would be appropriate then you will be directed to put this in).
Physiotherapist Contact Details
Sarah and Rosy are contactable by phone:
Telephone: 0300 1255152
If you have concerns about your child’s motor skills and they are not currently known to our service then you can request a referral via your Paediatrician, GP or the school health nurse.
Therapists work jointly work with other services to offer the following clinics.
Orthotics Clinic
The Orthotics clinic is for reviewing lower limb orthoses such as foot splints, gaiters, boots, insoles and helmets.
Orthotics clinics are ran on a Tuesday morning, every 2 weeks, by an Orthotist from North Bristol NHS Trust.
This is Ana Machado Rodrigues, Orthotist who is allocated to New Siblands School, from North Bristol NHS Trust.

Orthotics Referral Process
- In the first instance, speak with your child's class teacher or contact Kerry Purnell (Leader for Physical Disabilities)
-
Kerry Purnell will add the pupil onto the next available clinic if they are on the Orthotics caseload.
-
If the young person is not on the Orthotics caseload then a Kerry Purnell will liaise with the class teacher, parents and carers to complete a referral.
-
Kerry Purnell will liaise with with Orthotist in advance of the clinic to share the input required for the young person.
Orthotics Contact Details
To check on provision of Orthotics you can contact the orthotics department directly on 0300 300 0110.
They are now based at Highwood Pavillions in Patchway (The Enablement Centre, Cribbs Causeway near to Jump Softplay Centre)
Orthopaedic Clinic
These clinics run biannually in school with Mr Guy Atherton, Consultant Orthopaedic Surgeon, for children who are known to the physiotherapy team and are organised by Sarah Padwick. If your child needs to see Mr Atherton outside of the clinic time please discuss with your physiotherapist who will liaise with Sarah (if your child is not open to Sarah) to decide if your child should either be seen at the Children’s hospital or in a community clinic. Please note if your child needs an x-ray they may have to be seen in Mr Atherton’s Children’s Hospital clinic.
If your child has orthopaedic needs outside of the annual clinic, they can be reviewed in one of the clinics run at Patchway Hub or Bristol Children’s Hospital.
Rebound Therapy
Rebound Therapy: What is it?
The essential value of the process is that, for a brief moment ‘earth’ is left behind and a new freedom is found in controlled movement away from gravity’s straitjacket, in a sort of relaxed ‘poetry of motion’ available to all, irrespective of any disability.
Rebound Therapy is used to facilitate movement, promote balance, promote an increase or decrease in muscle tone, promote relaxation, promote sensory integration, improves fitness and exercise tolerance and to improve communication skills.
Rebound is a cross curricular vehicle to enhance learning in all curriculum areas because it is so enjoyable concentration and willingness to learn is hugely increased.
Time is spent assessing the needs of each child in collaboration with the class teacher to work towards set targets. A programme will then be planned and delivered to meet these goals. Identified pupils work 1:1 on the trampoline for a set amount of time through the academic year
This is Jane Hawkes.
Jane works one day a week at New Siblands. She works across both Primary and Secondary Sites delivering Rebound Therapy

School Nurse
This is Mel Coombs.
Mel is one of the School Health Nurses who is based in Patchway Hub Tuesday to Friday, all year round. She is no longer solely based in school.

More about the School Nurse
Mel Coombs has worked as the School Health Nurse for Special Schools since May 2012. I have over thirty years children’s nursing experience with a background in Neurosciences at Great Ormond Street, General Paediatrics and NICU at Southmead Hospital in Bristol and in Burns and Neurosciences at Frenchay’s Barbara Russell Children’s Unit.
During your child’s journey through school the School Nurse can help ensure that your child has access to the most appropriate health care and support. Children are eligible for this service after they enter Reception class at school and have undergone at least 12 weeks intensive toilet training once Toileting Recommendations have been issued by School Nursing. They also need to have an EHCP in place.
While your child is in Nursery School their Health Care Professional will continue to be their Health Visitor. The School Nurse will take over from them when they enter Reception.
The School Nursing Team can help with a number of issues as shown in the poster below.
There is information below about how to refer to the School Nursing Team.

Toileting
Preparing for Toilet Training
One of the best things we can do for our children is to teach them to be able to use the toilet appropriately and increase their independence and self-esteem. All staff in our school will fully support toilet training at all stages.
Toilet training is not just about coming out of nappies, pads and continence protection. It includes a wide range of skills a child needs to become reliably clean and dry and acquire reliable control of their bowel and bladder.
The earlier you start teaching your child to sit (nothing more at this stage) and feel comfortable sitting on the toilet or potty as part of their regular bedtime and morning routine, the better. It does not matter at this stage if they cannot use it to do a wee or a poo, just that they can start to sit on it without a nappy for a minute or two at a regular time, two or three times a day.
Once this routine is being accepted happily, toilet training can begin. Please try to start introducing this routine as early as you can. It is never too early to start and you may need to think about simple adaptations to the environment to help your child, such as a small step, a more secure toilet seat, a bag of toys to help occupy the time spent sitting and some visuals and maybe even a timer to measure the time. Always consistently use the phrase “toilet time” during this routine and do not expect any appropriate use of the toilet or to see signs that your child is aware of the process. If they do have an awareness, that will speed up the toilet training process but it is not unusual for this to come much late.
The most important thing at this stage is the routine of sitting. Any delay in starting them to sit regularly as part of a routine (like teeth cleaning and bathing) will delay the toilet training process. Give plenty of praise for just sitting on the toilet.
Toilet Training
Toilet training is an important milestone for your child, but learning to gain control of the bowel and bladder is a complex process and your child needs to be emotionally and physically ready to start formal toilet training. To help our children become emotionally and physically ready it is important to remember that the earlier toilet preparation is started, the easier the skill will be acquired. Any delay in the preparation will delay formal toilet training. Remember the Mantra: “All things toilet, stay in the toilet” for example only changing a nappy in the toilet (and not in the bedroom or anywhere else) can help the child register that this is where wee and poo should go.
Another thing that helps your child to understand is to always allow them to see that the contents of a dirty nappy (not the actual nappy or wet-wipes) are put down the toilet and flushed away. It can also help for your child to be able to see you use the toilet too.
During this time it is also important to ensure that your child has plenty of fluids during the day time and try to keep bedtime drinks to a minimum. If you notice that your child suffers from constipation, now is a good time to obtain some treatment from your GP. Constipation will also delay toilet training and impede any progress. Please see further advice regarding constipation later in this article.
Formal toilet training begins as a gradual process of increasing the sitting times that your child has already become used to as part of their normal bedtime and morning routine. This will include a mixture of starting to introduce sitting on the toilet after meals. The sitting times should be increased gradually from a couple of minutes to 5 minutes at a time. You may need toys, timers, social stories etc to occupy them help and focus the mind. Get your child used to this new routine and let everyone involved in the process know what words or signs your child makes if they want the toilet.

Raising Awareness
If your child uses disposable nappies, they may never feel wet or uncomfortable. Feeling wet and uncomfortable is an important part of the toilet training process. It helps children connect weeing with feeling wet.
If your child is happy so far with the toileting process and will happily sit on the toilet as part of their normal routine, it is time to introduce some discomfort. This is normally achieved by firstly putting kitchen roll inside the nappy. You can regularly check if they are wet and ask them to tell you when they are wet. You only need to do this during the daytime for the moment. If it does not seem to be having much effect then try this for one week out of every month. If it does seem to be having an effect, then continue for a period of two weeks at a time.
This may be the time to involve your child in buying some pants of their own and putting these on underneath their nappy instead of the kitchen roll. Continue to change them standing up if possible as this enables them to take an active part in the process: pulling pants up and down and learning to wipe their bottom themselves. Encourage them to wash and dry their hands and dress themselves. It is helpful to regularly read stories to them about using the toilet. Make sure that boys are always taught to sit down for both wees and poos and not encouraged to wee standing up. Standing can lead to delayed use of the toilet for poos and constipation in some cases.
Make a note of when your child is regularly weeing and pooing by checking the nappy every hour for a few days. Based on this pattern, you can take you child to the toilet at scheduled times. Blowing bubbles can help your child stay busy while on the toilet and also may help them to have a bowel movement too.
Once your child has a regular sitting routine in place and can stay dry for two hours they can stop using nappies. You can use washable training pants if required or their own underwear with waterproof pants over the top. You will need to keep a bag handy with a change of clothes, some wet-wipes for cleaning and seat protectors for school transport to send into school. Accidents are a normal part of the toilet training process so it is best to be prepared in advance.
Your child will gradually start to understand and know how to react and respond to the feeling that they need to empty their bladder or bowel. They will also need to understand what you want them to do and how to do it. It can take a long time but with regular routine and patience it can be achieved.
Constipation
Constipation must always be treated before any formal toilet training is started. It is very difficult for a child to have any control over his or her bladder if they are at all constipated. Constipation is very common in children and for many there is no known reason why it happens (this is known as idiopathic constipation). Research has shown that 29% of 4½ year olds and 27.5% of 9½ year olds in the UK suffer with constipation.
A child is considered to be constipated if they poo less than 3 times a week. However, every child’s pooing pattern is different and some children will need to poo twice a day whilst others will go only every other day. Recent evidence has found that constipation is very under-estimated as a medical condition. The best thing to aim for is a “soft daily pooh”.
Coping with constipation and soiling
In 2009 100,000 children in the UK were treated by their GPs for constipation and soiling problems. For most children, constipation can be successfully resolved. It can be a long journey, needing on-going support from health professionals and much patience and encouragement from parents and carers. The quicker a child has an assessment by their GP, the easier it will be to manage and resolve the problem.
Causes of constipation
- Withholding poo/ stool withholding (avoiding going to the toilet) – see more below
- Fear of the toilet (sometimes associated with pain or discomfort)
- Lack of a toilet routine (some children have such busy lives that it can be difficult to find time to sit and relax on the toilet each day
- Resistance to toilet training and an insistence that a nappy be put on to poo in
- A diet that is not fully balanced
- Low fluid intake
- A change in routine
- Anxiety and emotional upset
- Some medications may cause constipation
- Illness
- Withholding poo/ stool withholding
Stool withholding is when a child feels the need to use the toilet but resists it. Resisting the need might involve crossing the legs, sitting on the back of the heels, clenching the buttocks and being fidgety. The stool gets bigger the longer the child holds on to it and eventually when they absolutely have to go it is very painful and difficult to pass. This can lead to a vicious cycle of holding on and pain.
A child might start withholding stools for several reasons – they may have experienced passing a painful or difficult stool; they may have a sore or anal fissure which makes pooing painful; or they might not want to use strange or smelly toilets and prefer to hold on until they get home.
Recognising the signs of constipation
- Poo looks like hard pellets, maltesers or very large poos
- Soiling
- Unhappy, angry or irritable mood
- Regular and foul smelling wind
- Foul smelling poo
- Painful tummy
- Distended tummy
- Pain when pooing
- Pooing less than three times a week
- Straining
- Withholding poo
- Poor appetite
- Lack of energy
The Bristol Stool Form Scale can help you identify whether poo is becoming constipated. The ideal poo is number 4 on the scale – a soft, smooth sausage shape.
Establishing a routine
The pace of life can be so busy that it is easy to neglect the need to ensure there is time in the day for children to have a relaxed sit on the toilet for a poo.
Putting a toilet routine in place will ensure that sitting on the toilet for a poo is a regular part of a child’s day and will encourage the complete emptying of the bowel on a regular basis, helping to lessen pooing accidents and avoid constipation.
A toilet routine is especially important for boys who, once they begin to stand up to wee, have to make a special effort to sit on the toilet for a poo and pooing can become rushed or simply forgotten. Tips for successful pooing on the toilet The correct way to sit on the toilet to have a poo Tips on what to do when a child prefers to poo in a nappy
Soiling
What is soiling?
Children soil when they poo in their pants, on the floor or in other inappropriate places. Some children have a more regular and persistent difficulty.
Why soiling happens
Constipation is the most common cause of soiling. When children don’t poo regularly, the bowel can become loaded with large poos that are hard to pass. This is sometimes called faecal impaction.
Poo can appear runny (like diarrhoea), in small lumps or can be visible around the bottom and difficult to wipe away. Soiling occurs when runny poo leaks around the hard lump that is blocking the way; or if there has been a longstanding problem of constipation the lower bowel and rectum may have become overstretched. Soiling can happen several times a day as the child does not always receive the message that they need a poo or is not always aware that the poo has come out.
Treatment for constipation and soiling
Most parents seek help initially from their health visitor, school nurse or GP. Keeping a record of how often pants are soiled, poo is passed in the toilet and the type of poo passed will help health professionals assess the problem and offer appropriate intervention.
Treatment is likely to include:
- Medication to relieve constipation and clear faecal impaction (this is likely to be Movicol but could be a stool softener, stimulant laxative or bulking agent). The medicine is then continued to ensure that the poo remains regular and easy to pass, stopping the medication too soon can result in the constipation building up again
- Suggestions for appropriate changes to the diet and fluid intake
- Establishing a regular routine of sitting on the toilet for a few minutes at least once a day, 15-20 minutes after a meal
- Checking that your child is positioned comfortably and securely on the toilet (using a child seat if necessary), and ensuring that feet are firmly on the floor or supported on a step will help your child push poo out
- Teaching your child the technique of gently rocking forwards and back when sitting on the toilet
- Motivating your child by involving them and offering simple rewards for achieving targets
- Occasionally psychological help is useful to explore anxieties or stress that may be associated with, or aggravating the problem
Always consult your GP if your child is showing signs of constipation or there are changes in bowel patterns.
There is a lot of advice available and I would recommend ERIC at http://www.eric.org.uk/ and Promocon at http://www.disabledliving.co.uk/Promocon/Publications/Children/Toilet-Training
Sleep
Sleep Tips
A Contact-a-Family survey found that disabled children are more than twice as likely to have problems with sleep as others.
Without specialist support, sleep problems can continue for years. Sleep deprivation not only affects a child’s learning, behaviour, mood and health but also the physical and mental well-being of the whole family.
Some sleep problems are common with certain impairments, so you need to take account of your child’s diagnosis. But the large majority of sleep problems are behavioural, so there’s a lot you can do. Have a look at the following list and see if you can identify why your child may be having sleep difficulties.
Bedroom environment
Environment is one of the common reasons children have difficulties sleeping.
Room temperature
Is your child too hot or too cold? Ideally the temperature in the bedroom should be between 16–18 C.
An over-stimulating bedroom
Does your child get out of bed to play with toys? If so, your child may be over-stimulated by the bedroom environment. Bright colours are often stimulating to children. You will need to consider creating a restful bedroom environment. It’s important that your child’s bedroom is a calm and suitable environment for them to get to sleep in.
Screens
Is your child playing computer games or watching TV before they go to bed? Light from screens (such as tablet computers, mobile phones and TVs) blocks melatonin production. We recommend no screens the hour before bed. Use the settings control to automatically set night time settings to your phones and tablets. This ensures that a lower level of light is emitted during the evening.
Comfort
Is their bed comfortable? Try lying on it and seeing how it feels. Is your child wet or soiled? This will cause discomfort which could impact on their ability to sleep.
Bedding
Is your child kicking the bedding off during the night and waking because they are cold? If so, you can consider using a double duvet tucked under the mattress of a single bed. Or are they too hot or too cold, think about what you are experiencing at night time. If you are sleeping with just a sheet on, and your child has a heavy duvet, they could be getting too hot.
Noise
Is there any noise inside or outside the home that may be disturbing your child? Some children with sensory issues, such as autistic spectrum disorders, can be particularly sensitive to noise. What may seem like a quiet sound to you can seem very loud to them. The noise of an electric fan can mask other noises in your home and may be worth considering if noise is an issue.
Light
Is the room dark enough? Melatonin is produced when the room is dark. You might consider buying black-out blinds to make the room darker.
Hunger
Could your child be hungry? What time are they having their tea-time meal? Does their meal-time need to be later? Giving your child a snack mid-afternoon can help if you want to try moving their meal-time to later in the day. There are also foods that can help at bedtime.
Thirst
Is your child using ‘I’m thirsty’ as a distraction technique, or are they genuinely thirsty? Monitor what they are drinking during the day and give them a drink with their bedtime snack. Try offering water at night time, instead of juice or milk. If they are thirsty, they will drink water.
Lack of understanding about day and night
Does your child understand the difference between day and night? Sometimes children with additional needs require help to learn when it’s daytime and when it’s time to sleep, particularly if they have a visual difficulty. Tried and tested strategies can help with this. The same sequence of events should happen every night. Visual or other timetables can help a child understand the order of events and what is going to happen next. Gro Clocks can help too. Search for them online.
Bedtime routine Does your child’s bedtime routine encourage sleep? Has their routine become unsettled lately because of an event like a family holiday or Christmas?
Getting up too early
If your child wakes in the night do you treat it as a night awakening, or as the start of the day? You should consider what a reasonable time to begin the day is. If your child wakes before that time, return them back to their bed. This will help to strengthen their body clock.
Pain
Is your child in pain? Could they be teething? Some disabled children cannot reposition themselves at night which can disrupt their sleep. If you think that your child may be in pain you should seek advice from medical professionals.
Medication
Is your child on any medication that may affect their sleep? Or do they have to be given medication during their sleep which may be disturbing them? Check with a medical practitioner if you are unsure.
Sleep Routine
Wind down
An hour before bed, turn off the TV and all other screens (such as iPad, games consoles and phones), dim the lights and close the curtains to begin the visual clues it’s coming up to bedtime.
Drinks Avoid drinks of cola and chocolate at bed time. Have a sleep food snack to help your child with their sleep.
Bath time
Half an hour before bed, it’s bath time. If your child finds a bath too stimulating, bath earlier in the evening. On a non-bath night, a cuddle in a warm towel will help.
After the bath it’s time to brush teeth and get ready for bed (put on pyjamas).
Quiet time before sleep
- Sit with your child and spend half an hour of quieter fine finger games (such as playing with jigsaws, colouring, drawing, threading, hammer beads).
- Then it’s bathtime; don’t go back downstairs after you have gone to the bathroom.
- If your child finds a bedtime story calming, spend the next 5 minutes sharing a book, no stimulating storylines as this could have an adverse affect.
- Then it’s a kiss and cuddle goodnight, and leave the room. Remember you want to leave them awake, so they fall asleep in the same conditions that will remain all night (alone).
- Wake your child every morning at a set time so they can learn the routine and you can help strengthen their body clocks.
Sleep Diary
When we are sleep deprived, we can become forgetful and stressed so don’t always recognise what’s happening at night.
Every night merges into one, so you need to be able to take night time and look at it in segments. Using a sleep diary can help you identify areas of inconsistency, areas to praise or perhaps you might notice your child is getting more sleep than you thought! Download a sleep diary
Tips for using a sleep diary
- You need to complete your sleep diary honestly to use it effectively. Use extra sheets if you need to.
- If your child sleeps elsewhere, such as a respite centre or another family member’s house, ask them to fill in the sleep diary. You might notice your child sleeps better there and using the diary will be able to identify why.
- Check with your school to see if your child naps in the day, or with the escort if they travel home by bus. This will affect night time sleep if the nap is too late in the day or if they are at an age where naps are not appropriate.
- Keep the diary by the bed with a pencil so that you can fill it in immediately rather than trying to remember what happened later.
- Share the diary with professionals who work in sleep to see if they can help you find a cause for your child’s sleeping difficulties.
- Keep the diary for at least two weeks and then see if you can identify a pattern to your child’s sleeping habits. You can then identify an area that you can start to address.
Sleep-inducing Foods
Experiment with your child’s food intake to find the right amount of food to have in the evening. It takes around one hour for the tryptophan in foods to reach the brain, so don’t wait until right before bedtime to have your snack.
Whole-wheat bread
A slice of toast with your tea and honey will release insulin, which helps tryptophan get to your brain. Once there, tryptophan turns into serotonin – which murmurs: “time to sleep”.
Bananas
They’re practically a sleeping pill in a peel! Bananas contain a bit of soothing melatonin and serotonin, as well as magnesium, a muscle relaxant.
Honey
Drizzle a little in your warm milk or herb tea. Lots of sugar is stimulating. But a little glucose tells your brain to turn off orexin, a recently discovered neurotransmitter linked to alertness.
Warm milk
It’s not a myth. Milk has some tryptophan – an amino acid that has a sedative-like effect – and calcium, which helps the brain use tryptophan. Plus there’s the psychological throw-back to infancy, when a warm bottle meant “relax, everything’s fine”.
Oatmeal
Oats are a rich source of sleep-inviting melatonin. A small bowl of warm cereal with a splash of maple syrup is cosy – and if you’ve got the munchies, it’s filling too.
Almonds and peanut butter
A handful of these heart-healthy nuts can be snooze-inducing, as they contain both tryptophan and a nice dose of muscle-relaxing magnesium.
Potatoes
A small baked spud won’t overwhelm your digestion, and it clears away acids that can interfere with yawn-inducing tryptophan. To increase the soothing effects, mash it with warm milk.
Turkey
It’s the most famous source of tryptophan, always credited for all those Christmas naps. But that’s modern folklore. Tryptophan works when your stomach’s empty, not overstuffed, and when there are some carbs around, not tons of protein. So put a lean slice or two on some whole-wheat bread mid-evening, and you’ve got one.
Clinics
Paediatricians Clinics
Dr Julianne Dare, Consultant Paediatrician, holds a morning clinic every 2nd Thursday of the month in school.
Approximately 80 Paediatrician clinic appointments are offered per year at New Siblands. It is very important to attend your appointments in school and if you cannot attend please let the bookings clerk know so they can offer that appointment to someone else on the waiting list. Parents do have to attend for the appointment to take place.
School Nurses are no longer involved in the Paediatrician’s clinics; Paediatricians now have their own clinic assistant who will attend the clinic to do heights and weights.
COVID Update:
All clinics are currently being held via Telephone
School Nursing Drop-In Clinics
Parents can contact the School Nursing Service for advice and information any time on 01454 862442.
COVID Update:
Due to the current pandemic, these clinics are currently on hold at this present time.
Community Eye Team
Orthoptic Clinics are held by with Julie Parker. The Optometrist will holds Optometry Clinics every term usually and Kerry Purnell (Leader for Physical Disabilities) coordinates this. School Nurses are no longer involved in the Community Eye clinics.
Immunisation clinics
School immunisations occur in school and are delivered by the Sirona Immunisations Team throughout the year: You will be sent consent forms which need to be returned to school.
- Seasonal Influenza (‘Flu) Vaccine nasal spray will be available from October for all pupils up to and including those aged 17 years of age.
- Meningitis ACWY vaccine for all Year 9 pupils
- Tetanus, Diphtheria, Polio teenage booster for all Year 9 pupils
- HPV Preventing Cervical Cancer for all Year 8 and Year 9 pupils, first dose in year 8, second in year 9. This extends to boys from September 2019.
Special Needs Dentist
The School Health Nurse can make a referral to the Special Needs Dental Department in Yate if you would like to be seen there.
The school does NOT have its own dentist but the Special Needs Dentist occasionally carries out Dental Screening. This is for statistical purposes only and does not include any treatment.
The Special Needs Dental Department in Yate do not send out 6 monthly reminders so you need to ensure that you make a future appointment before you leave the department.
School Nurse Referral Process
- If you would like to be referred to the School Health Nursing Team, you can liaise with you child's class teacher who will complete a School Nurse request for support form. Alternatively you can self refer as a parent.
- The referral form is available from the CCHP website: https://cchp.nhs.uk/cchp/explore-cchp/school-health-nursing/school-nursing-information-resources or it is attached at the bottom of this page.
- This referral is emailed to Sirch.southglosschoolnursing@nhs.net who will respond to the referral, contact the parent/carers and update the referrer.
School Nurse Contact Details
New Siblands School Link Nurse is Mel Coombs. You can contacted via:
Email: sirch.southglosschoolnursing@nhs.net
Telephone: 0300 125 5151
Letter: Patchway Hub, Patchway locaality hub, Rodway Road, Patchway, BS345PE, marked for the Attention of Mel Coombs
Speech and Language Therapy
Enable Trust has the vision of ‘Working together passionately to achieve the best outcomes for our SEND children and young people’.
At New Siblands and Culverhill we have the ambition to meet children’s needs better (including meeting SEMH needs) more successfully.
During the academic year 2022/2023 Enable Trust schools reviewed their therapeutic provision and have created a Speech and Language Therapy (SALT) Team. As Enable Trust and Therapy Team expand a workable model is being developed which will grow in readiness for a longer term sustainable way of working and therapy provision which can provide outreach opportunities outside the Trust.
Jane Stonehouse is the Lead Speech and Language Therapist and Michelle Jefferies is the Assistant Speech and Language Therapist for Enable Trust. They work across Two Bridges Academy, New Siblands School and Culverhill School during the week.


The Core speech and language therapy service, provided by NHS, works in collaboration with educational settings and they will support students with high level AAC needs and eating and drinking difficulties.
The core speech and language therapist allocated to New Siblands School is Rachel Humphries and Paula Saint is the speech and language therapist Assistant Practitioner. Rachel and Paula will be based at New Siblands on a Thursday and will liaise directly with Jane Stonehouse to identify students to support in line with the NHS service offer.


The Enable Trust Speech and Language Therapy (SALT) Team may support children in the following areas:
- Developing pupil’s language and communication skills.
- Developing alternative methods of communication e.g. Makaton signing, communication books, PECS, high tech communication aids etc
- Developing pupil’s social communication skills.
- Developing pupil’s speech sound production.
- Developing fluency when talking
- Developing pupil’s eating and drinking skills and assessing the safety of their swallow.
The SALT Team are able to assess individual pupil’s speech, language and communication skills when appropriate. Following this, advice and recommendations are provided to help the pupil’s develop their areas of need. They will see pupil’s to provide SALT provisions as detailed in their EHCP’s.
The SALT team also work very closely with the teaching staff to ensure that:
- Explicit communication and interaction approaches are embedded in every lesson.
- Practical SALT activities are embedded in most lessons across the curriculum.
These are crucial aspects of our work within Enable Trust Schools because progress with communication and interaction skills requires daily inputs and these are most effective when delivered within the school curriculum.
Children may be seen in school for therapeutic SALT interventions, either individually or in groups. In addition, for some pupils, SALT interventions and programmes of work are delivered by school staff under direction and oversight from the Speech & Language Therapy Team.
The Enable Trust SALT model has been devised to show the offer for all students. Each students needs will be assessed and they will be assigned a tier. The below shows the level of input they require by class team and SALT. As both New Siblands and Culverhill are specialist schools this provision could look quite different to mainstream ways of working. Many aspects of our SALT provision are delivered in class as part of our total communication approach.
|
Tier 1 Needs met by whole class communication approach Class team led with input from SALT team
Access to a specialist language rich curriculum where SALT is regularly involved in planning and review. SALT to support CPD of Teaching staff in order to meet pupil needs Speech and Language Pedagogical techniques embedded in curriculum Ability to seek advice about any initial language concerns Communication strategies implemented by class team in the classroom Functional communication system in place Visuals Use of makaton Objects or reference used in classes where appropriate |
|
Tier 3 Direct input from SALT
New students Brief report towards EHCP following direct work or change of provision on EHCP Dysphagia Block sessions/ weekly 1:1 session with SALT as specified and quantified on EHCP Significant change of need where concerns of impact to mental health, wellbeing or behaviour or student needs a SALT review Termly reviews of progress with SALT Feeding needs including sensory New communication system Child with no functional communication system
|
|
Tier 2 Input from SALT team with oversight from SALT
Daily/ weekly/ block sessions led by SALT assistant/ specialist SALT TA or Class Team with oversight by Therapist Programme / communication system up and running and implemented within the class, with regular review from SALT assistant/ specialist SALT TA Previous block of intervention in Tier 3 and need to consolidate Update targets at the end of long term (3 times per year) Low risk sensory feeding (e.g food groups) |
|
Tier 4 External specialist SALT for highly specialised support |
Speech and Language Therapist Contact Details
Jane is contactable by phone or email Monday - Thursday:
Jane.Stonehouse@enabletrust.org.uk
Telephone: 01454 553002





